Fertility Specialist Clinician Appointment
All our clients are required to make an appointment with one of our Specialist Clinicians to discuss their specific requirements, undergo medical assessment and screenings, receive counselling and have their questions and concerns answered. Following this consultation a personalised treatment plan will be arranged for them to enable the best outcome.
Inspire IVF staff are approachable to answer any subsequent questions and will keep our clients fully informed of their progress during their treatment cycle.
What is IVF?
The term In vitro fertilisation, IVF, literally means fertilisation “in glass” and refers to the process where a woman’s eggs are fertilised outside of her body in the laboratory. The resulting embryos are then transferred back into the uterus a few days later or frozen and stored for future use.
Indications for IVF include prolonged unexplained infertility, endometriosis, the treatment of male factor problems with intra-cytoplasmic sperm injection (see ICSI) and more recently to reduce the chance of transmitting a hereditary or genetic disease. (see PGD).
Who is standard IVF suitable for?
IVF is specifically recommended for women with absent, blocked or damaged fallopian tubes. The male should have normal sperm parameters – good numbers, good motility and good morphology. It is also often used in cases of unexplained infertility.
Who is ICSI suitable for?
ICSI is used to treat infertility related to poor sperm quality and / or quantity, for older women, patients with previous IVF failure, and patients who are to undergo PGS/PGD.
What does the procedure involve?
The steps involved in an IVF cycle are:
- Stimulation of the ovaries to encourage development and maturation of the eggs.
- Retrieval of the eggs
- Collection and preparation of the sperm sample
- Fertilisation of the eggs and culture of the embryos
- Transfer of the embryos back into the uterus
- (Biopsy and Preimplantation Genetic Diagnosis/Screening if indicated)
OVARIAN HYPERSTIMULATION
Controlled Ovarian Hyperstimulation (COH)
Stimulation of the ovaries to encourage development and maturation of eggs Under the care of a Fertility Specialist, the woman is given fertility medications to stimulate her ovaries to produce many follicles. Follicles are the small fluid filled structures which develop on the ovaries, each of which will hopefully contain an egg. The number and size of the developing follicles is measured by trans-vaginal ultrasound scan monitoring. The exact number of follicles which develop varies between patients, depending on age and aetiology. The final preparation for egg retrieval involves a hormone injection (Trigger Shot) which mimics the natural trigger for ovulation. Egg retrieval will take place 36-38 hours after this injection.
Retrieval of the Eggs
Trans Vaginal Oocyte Aspiration (TVOA)
Egg retrieval is a procedure which is carried out under light anaesthesia in our operating theatre. A trans-vaginal ultrasound probe is used to visualise the ovaries and a needle attached to the probe is passed through the vaginal wall into the follicles. The fluid within each follicle is aspirated and then examined in the IVF laboratory for the presence of an egg. After identification, the eggs are washed and transferred into culture medium in special dishes in an incubator.
Fertilisation of the eggs and culture of the embryos
While the egg retrieval is proceeding, the sperm is also prepared. A semen sample is provided by the male partner and, in the laboratory, a concentrated preparation of the best motile sperm is extracted from the semen sample.
In a Standard IVF procedure this sperm preparation (containing a calculated number of sperm) is added to the dishes containing the eggs, and they are incubated together overnight.
ICSI is a procedure which involves injecting a single sperm into each egg using a very fine needle, rather than mixing the eggs and sperm in a dish (see Intra Cytoplasmic Sperm Injection)
Irrespective of the method of insemination used, on the morning after egg retrieval, the eggs are examined to see which have fertilised.
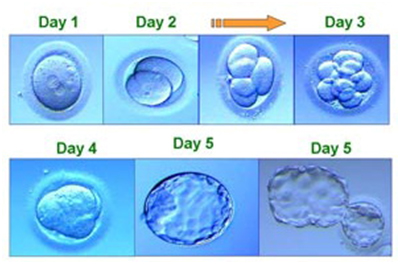
Fertilised eggs (zygotes) are routinely cultured in the IVF laboratory until at least day 3, in most cases embryos are grown to day 5 or 6 (Blastocyst), at which time the best 1 or 2 embryos are selected and transferred back into the woman’s uterus.
Inspire IVF generally recommends that patients culture embryos to Day 5 or 6, where embryo biopsy can take place, at the client’s request, and subsequent screening of the embryo can be done for genetic and hereditary diseases. The decision to have testing of embryos will be made in consultation with our fertility clinicians so our clients receive counselling and are fully informed of their options.
Transfer of the embryos into the Uterus (ET – Embryo Transfer)
The embryo transfer cycle is relatively non-invasive procedure. The embryos can be replaced either in a natural cycle or in a controlled medicated cycle. We aim to transfer the embryos into the uterus at the correct time in relation to ovulation and the thickness of the lining of the uterus (endometrium). Often this is done by using ovulatory medication to better time the transfer.
For most women it is very much like having a pap smear. One or two embryos are loaded into a fine catheter, which is passed through the cervix and into the uterus under ultrasound guidance. The embryo/s are then gently expelled.
Any additional suitable embryos that are not transferred fresh can be frozen for the client’s future use in a Frozen Embryo Transfer Cycle (FET).
How will I feel?
The drugs used in the controlled ovarian hyperstimulation stage of the procedure are designed to “hijack” your normal menstrual cycle and force the ovary to produce several instead of 1 egg. Any symptoms that you associate with your normal cycle will be exaggerated by this process.
Other symptoms such as hot flushes and dizziness are common in the early stages whilst some lower abdominal pain, bloating and tiredness are common after the TVOA.
What are the risks involved?
Controlled Ovarian Hyperstimulation (COH)
The main risks associated with stimulation arise from either too much or too little stimulation.
Too much gives rise to a complication called Ovarian Hyperstimulation Syndrome (OHSS). In this, over sensitivity to the drugs used causes so many eggs to develop that they produce such high levels of circulating hormones, that they become toxic. To protect against this potentially dangerous situation any resulting embryos are cryogenically frozen, as pregnancy would make the condition worse and more prolonged. Particularly bad cases can result in the complete cancellation of a treatment cycle. Too little response to the drugs results in too few eggs. This sometimes also necessitates the cancellation of a cycle or the production of just a small number of eggs for fertilization.
Trans Vaginal Oocyte Aspiration (TVOA)
Whilst the egg pick-up procedure requires an anaesthetic, it is usually very light and has few associated risks, though some post operative nausea and dizziness are relatively common and transient. There may be some light vaginal bleeding and rarely, a pelvic infection occurs.
In-Vitro Fertilisation (IVF)
This laboratory based process has it’s own associated risks.
Laboratory Risk
While any system is susceptible to human error, Inspire IVF has introduced internationally accepted standards, the implementation a quality management system and the double checking/witnessing, on every sample at every step of the procedure. This is done to produce a fail-safe process, regarding mismatch of eggs/sperm/embryos. Similarly, high standards in equipment quality and maintenance are designed to minimize the risk of equipment failure and subsequent damage to stored eggs/sperm/embryos.
In the event of power failure Inspire IVF has a back up generator to ensure continuity of power supply, we utilise UPS systems and some equipment has it’s own battery back up.
Male partner risks
Provision of an unsuitable semen sample on the part of the male partner may necessitate either a repeat sample, or if that is not possible, an emergency surgical collection. This is obviously a rare event and is only an issue where there is a recognized semen problem. The male partner is encouraged to ejaculate frequently in the month leading up to TVOA, to ensure his sperm is of optimal quality.
Embryo Transfer (ET)
This is usually the easiest part of the whole IVF process and for most women is very much like having a pap smear. Some women can have narrowed or unusually shaped cervixes which can make the process more difficult and uncomfortable. Rarely failure to be able to get through the cervix can mean the procedure must be done under anaesthetic in the operating theatre.
In practical terms, twins as the result of the transfer of more than one embryo is the most common complication of this procedure. It is because of the increased risk associated with multiple pregnancies to both the mother and babies.